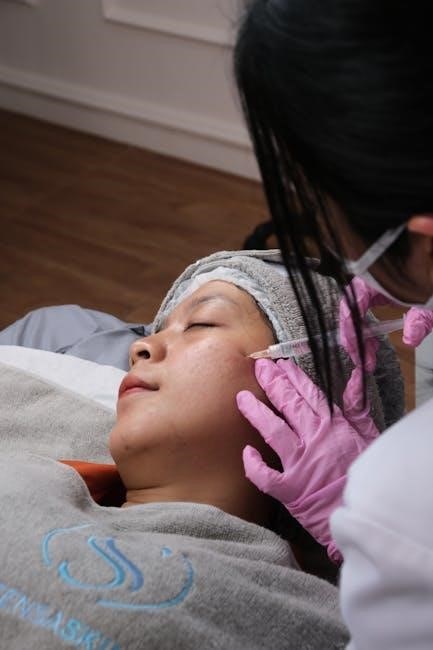
Equine Joint Injections: A Comprehensive Guide (Updated 03/09/2026)
This guide, informed by equine surgeon Thijs de Bont MRCVS, details joint injections for pain and performance management in horses, offering clarity on their use.
Equine joint injections represent a cornerstone of modern equine orthopedic medicine, offering targeted relief for pain and improved performance. As detailed by equine surgeon Thijs de Bont MRCVS, these injections deliver medication directly into the affected joint, minimizing systemic side effects. This approach is crucial for managing a variety of conditions, from the subtle discomfort of early osteoarthritis to the more pronounced pain associated with acute injuries.
This comprehensive guide aims to demystify the process, covering everything from understanding joint anatomy and disease to exploring the diverse range of injectable medications available. We will delve into diagnostic procedures, injection techniques, post-injection care, and potential complications, providing horse owners and professionals with the knowledge needed to make informed decisions.
Understanding Equine Joint Anatomy & Disease
A thorough grasp of equine joint anatomy is fundamental to understanding the rationale behind joint injections. Equine joints, like those in humans, are complex structures comprised of bone, cartilage, ligaments, and synovial fluid. Cartilage provides a smooth, low-friction surface for movement, while synovial fluid nourishes the cartilage and lubricates the joint. Disease processes often target these components.
Common issues include cartilage damage, inflammation of the joint lining (synovitis), and the degenerative changes associated with osteoarthritis. These conditions disrupt the normal joint environment, leading to pain and reduced function. Understanding how these diseases affect the joint’s structure and mechanics is vital for targeted treatment, as highlighted by experts like Thijs de Bont MRCVS, and informs the selection of appropriate injectable therapies.
Common Causes of Joint Pain in Horses
Joint pain in horses stems from a variety of underlying issues, frequently requiring diagnostic investigation and, often, intervention like joint injections. Osteoarthritis, or degenerative joint disease, is a prevalent cause, resulting from cartilage breakdown over time, often linked to strenuous activity or previous injury; Synovitis, inflammation of the joint lining, can occur due to trauma, infection, or an autoimmune response.
Furthermore, direct cartilage damage – perhaps from a twisting injury – or meniscal tears within the joint can induce significant pain. These conditions disrupt the joint’s normal biomechanics, leading to lameness and reduced performance. As equine surgeon Thijs de Bont MRCVS notes, accurate diagnosis of the root cause is crucial for effective treatment planning.

3.1 Osteoarthritis (Degenerative Joint Disease)
Osteoarthritis (OA) represents a significant source of chronic joint pain in horses, characterized by progressive cartilage degradation. This isn’t simply “wear and tear”; it’s an active process involving enzymatic breakdown of cartilage matrix, leading to altered joint mechanics and bone remodeling. Initial stages may present subtle lameness, worsening with increased activity. As OA progresses, inflammation contributes to pain and reduced range of motion.
Factors accelerating OA include repetitive stress, conformational defects, and previous injuries. Equine surgeon Thijs de Bont MRCVS emphasizes that managing OA focuses on alleviating pain, reducing inflammation, and supporting joint function, often utilizing joint injections as a key component of a broader treatment plan.
3.2 Synovitis (Inflammation of the Joint Lining)
Synovitis, or inflammation of the synovial membrane lining the joint, is a common cause of acute lameness in horses. This inflammation leads to increased production of synovial fluid, causing joint swelling, heat, and pain. Synovitis can stem from trauma (e.g., a bruise or strain), infection, or an underlying condition like osteoarthritis.
Equine surgeon Thijs de Bont MRCVS highlights that prompt diagnosis and treatment are crucial. Joint fluid analysis often reveals elevated cell counts and protein levels, confirming synovitis. Treatment aims to reduce inflammation and address the underlying cause, frequently employing joint injections containing corticosteroids or other anti-inflammatory medications to provide targeted relief.
3.3 Cartilage Damage & Meniscal Tears
Cartilage damage and meniscal tears represent significant sources of joint pain in horses, often leading to chronic lameness. Cartilage, the smooth surface allowing joint movement, can degrade due to trauma or osteoarthritis; Meniscal tears, injuries to the fibrocartilaginous structures within the joint, further compromise joint function.
According to equine surgeon Thijs de Bont MRCVS, diagnosis frequently involves advanced imaging like MRI. Treatment strategies vary based on the severity of the damage. Joint injections, utilizing substances like hyaluronic acid or PRP, aim to provide lubrication and stimulate cartilage repair. In severe cases, surgical intervention may be necessary to address the damage and restore joint stability.
Diagnostic Procedures Before Injection
Accurate diagnosis is paramount before administering joint injections, ensuring targeted treatment and maximizing efficacy. A thorough lameness examination, including flexion tests, is the initial step, often followed by nerve blocks to pinpoint the source of pain.
Advanced imaging plays a crucial role. Radiography (X-rays) reveals bony changes, while ultrasound imaging visualizes soft tissues like ligaments and tendons. Joint fluid analysis, or synovial fluid analysis, assesses for inflammation, infection, and cartilage breakdown. As equine surgeon Thijs de Bont MRCVS emphasizes, a comprehensive diagnostic approach guides appropriate injection selection and improves the likelihood of a positive outcome.

4.1 Lameness Examination & Nerve Blocks
The lameness examination forms the foundation of diagnosing joint pain, beginning with observation of the horse’s movement at walk, trot, and canter. Flexion tests are then performed, stressing specific joints to elicit a response.
When the source of lameness remains unclear, nerve blocks are strategically employed. Local anesthetic is injected near nerves supplying a region, temporarily blocking pain signals. This helps isolate the affected joint. As highlighted by equine surgeon Thijs de Bont MRCVS, careful and systematic nerve blocking, combined with a detailed lameness exam, is vital for accurate diagnosis before considering joint injections.
4.2 Radiography (X-rays)

Radiography, commonly known as X-rays, is a crucial diagnostic tool for evaluating equine joint health. They allow visualization of bony structures within and around the joint, revealing changes indicative of osteoarthritis, such as bone spurs (osteophytes) and subchondral bone sclerosis.
Multiple views are typically taken to provide a comprehensive assessment. As emphasized by equine surgeon Thijs de Bont MRCVS, while X-rays excel at showing bone detail, they don’t directly visualize soft tissues like cartilage or ligaments. Therefore, radiography is often used in conjunction with other imaging modalities to achieve a complete diagnostic picture before proceeding with joint injections.
4.3 Ultrasound Imaging
Ultrasound imaging provides a real-time, dynamic assessment of soft tissues surrounding the equine joint. Unlike radiography which focuses on bone, ultrasound excels at visualizing ligaments, tendons, and joint capsules. This allows for the detection of injuries like ligament strains, tendonitis, and synovial fluid accumulation.
As highlighted by equine surgeon Thijs de Bont MRCVS, ultrasound is particularly useful for guiding joint injections, ensuring accurate needle placement. It can also assess the quality and quantity of synovial fluid. While ultrasound doesn’t penetrate bone well, its ability to visualize soft tissues makes it an invaluable component of a comprehensive pre-injection diagnostic workup.
4.4 Joint Fluid Analysis (Synovial Fluid Analysis)
Synovial fluid analysis, often called joint tapping, is a crucial diagnostic step before administering joint injections. This procedure involves aseptically withdrawing fluid directly from the joint space for laboratory evaluation. Key parameters assessed include cell count, protein levels, and the presence of bacteria.
Elevated cell counts suggest inflammation, while increased protein levels can indicate joint damage. Identifying bacteria confirms infection. As equine surgeon Thijs de Bont MRCVS emphasizes, analyzing the fluid helps determine the underlying cause of joint pain and guides appropriate treatment decisions, ensuring injections are targeted and effective. It also rules out septic arthritis before injection.
Types of Joint Injections
Several injectable medications are utilized to manage equine joint pain, each with a unique mechanism of action. Corticosteroids reduce inflammation, providing short-term relief, while hyaluronic acid (HA) acts as a viscosupplement, improving joint lubrication. Polysulfated glycosaminoglycans (PSGAGs), like Adequan, promote cartilage health.
More advanced therapies include IRAP (Interleukin-1 Receptor Antagonist Protein), which modulates the inflammatory response, and PRP (Platelet-Rich Plasma) therapy, utilizing the horse’s own healing factors. Finally, stem cell therapy, though still evolving, aims to regenerate damaged cartilage. As highlighted by Thijs de Bont MRCVS, selecting the appropriate injection depends on the specific diagnosis and stage of joint disease.
5.1 Corticosteroids: Mechanism & Use
Corticosteroids are potent anti-inflammatory drugs frequently employed in equine joint injections to rapidly reduce pain and effusion. They work by suppressing the inflammatory cascade within the joint, decreasing the production of inflammatory mediators. While highly effective for short-term relief, their use requires careful consideration.
As noted by equine surgeon Thijs de Bont MRCVS, repeated or high-dose corticosteroid injections can have systemic side effects and potentially contribute to laminitis. Therefore, they are often used strategically in conjunction with other therapies, like hyaluronic acid, to manage inflammation while minimizing long-term risks. Precise dosage and injection technique are crucial for optimal results.
5.2 Hyaluronic Acid (HA): Viscosupplementation
Hyaluronic acid (HA) is a naturally occurring substance in synovial fluid, vital for joint lubrication and shock absorption. In equine medicine, HA is injected to supplement the existing fluid, a process known as viscosupplementation. This aims to restore the fluid’s viscosity, improving joint mechanics and reducing pain.
As highlighted by equine surgeon Thijs de Bont MRCVS, HA’s effects are generally slower to manifest than corticosteroids, but offer a more sustained benefit. It doesn’t directly address inflammation but improves the joint environment, promoting cartilage health. HA is often used as part of a comprehensive joint management plan, frequently combined with other injectables for synergistic effects and long-term support.
5.3 Polysulfated Glycosaminoglycans (PSGAGs) – Adequan
Polysulfated glycosaminoglycans (PSGAGs), commonly known by the brand name Adequan, represent a unique approach to joint disease management in horses. Unlike corticosteroids or HA, PSGAGs work by inhibiting the enzymes that degrade cartilage and promoting the production of new cartilage components.
As detailed by equine surgeon Thijs de Bont MRCVS, Adequan is typically administered as an intramuscular injection series, rather than directly into the joint. This systemic approach allows the drug to reach all joints, making it suitable for horses with widespread joint issues. While not providing immediate pain relief, PSGAGs aim to modify the disease process, offering a chondroprotective effect and improving long-term joint health.
5.4 IRAP (Interleukin-1 Receptor Antagonist Protein)
IRAP, or Interleukin-1 Receptor Antagonist Protein, is a biologically-derived therapy gaining prominence in equine joint disease management. As explained by equine surgeon Thijs de Bont MRCVS, IRAP utilizes the horse’s own blood to create a protein that specifically blocks the effects of interleukin-1 (IL-1), a key inflammatory mediator in joint disease.
The process involves drawing a blood sample, stimulating white blood cells in vitro, and then injecting the resulting IRAP solution directly into the affected joint. This targeted approach aims to reduce inflammation and cartilage degradation. IRAP is often considered for horses that haven’t responded adequately to traditional treatments like corticosteroids, offering a potentially longer-lasting and more natural anti-inflammatory effect.
5.5 PRP (Platelet-Rich Plasma) Therapy
Platelet-Rich Plasma (PRP) therapy is a regenerative medicine technique increasingly utilized in equine orthopedics, leveraging the horse’s own healing capabilities. Equine surgeon Thijs de Bont MRCVS highlights that PRP involves concentrating platelets from a blood sample – these platelets contain growth factors crucial for tissue repair and inflammation modulation.
The concentrated PRP is then injected into the affected joint, aiming to stimulate the body’s natural healing processes. PRP is thought to promote cartilage repair, reduce inflammation, and alleviate pain. It’s often employed in cases of mild to moderate joint disease, tendon or ligament injuries, and can be used in conjunction with other therapies. The benefits are derived from the growth factors released by the activated platelets.
5.6 Stem Cell Therapy – Current Status
Stem cell therapy represents a cutting-edge approach to equine joint disease, though its role is still evolving and under ongoing research. As highlighted by equine surgeon Thijs de Bont MRCVS, the therapy utilizes stem cells – cells with the potential to differentiate into various tissue types – to regenerate damaged cartilage and reduce inflammation within the joint.
Typically, stem cells are harvested from the horse’s bone marrow or adipose (fat) tissue, then processed and injected into the affected joint. The goal is for these cells to differentiate into chondrocytes, the cells responsible for cartilage production. While promising, stem cell therapy isn’t a guaranteed cure and its long-term efficacy is still being evaluated through continued studies and clinical observation.
Injection Techniques & Protocols
Successful joint injections hinge on meticulous technique and strict adherence to sterile protocols to minimize complications. Aseptic preparation is paramount, beginning with thorough skin disinfection using surgical scrub solutions. The veterinarian, guided by anatomical knowledge and palpation skills, precisely locates the joint space.
Needle selection is crucial, considering joint size and depth. Insertion typically occurs using a swift, confident motion, aiming directly into the joint capsule. Correct joint positioning, often involving flexion or extension, aids in accurate needle placement. Post-injection, the site is cleaned again, and the horse is monitored for any immediate reactions. Maintaining sterility throughout the process is non-negotiable for optimal outcomes.
6.1 Sterile Technique & Asepsis
Maintaining strict sterile technique and asepsis is absolutely critical during equine joint injections to prevent devastating complications like septic arthritis. This begins with the veterinarian thoroughly scrubbing the injection site with a surgical scrub, often utilizing chlorhexidine or povidone-iodine solutions.

The use of sterile gloves, syringes, and needles is non-negotiable. Preparation of the medication itself must occur under sterile conditions. Skin preparation extends beyond the immediate injection point, encompassing a wide surrounding area. Draping the limb with a sterile surgical drape further enhances the sterile field. Any breach in sterile technique immediately compromises the procedure and increases infection risk.
6.2 Joint Positioning & Palpation
Accurate joint positioning and skillful palpation are fundamental to successful and safe equine joint injections. Proper positioning ensures optimal access to the joint space while minimizing the risk of injecting surrounding tissues or structures.
The veterinarian will carefully palpate the joint to precisely identify key anatomical landmarks – bony prominences and ligamentous structures – guiding needle placement. This often involves flexing or extending the limb to better define the joint capsule. Consistent and accurate palpation minimizes the chance of injecting into unintended spaces, like tendon sheaths or muscle. Experienced practitioners rely heavily on tactile feedback to confirm correct needle positioning before injecting.
6.3 Needle Selection & Insertion
Choosing the appropriate needle gauge and length is crucial for successful joint injection. Generally, a 22- to 25-gauge needle is utilized, balancing ease of insertion with sufficient rigidity for accurate placement. Needle length depends on the joint size and the horse’s conformation; typically ranging from 1.5 to 3.5 inches.
Insertion requires a steady hand and a deliberate approach. The skin is prepped aseptically, and the needle is advanced at a shallow angle, guided by palpation. A ‘pop’ or decrease in resistance often indicates entry into the joint space, but aspiration is always performed to confirm. If no synovial fluid is retrieved, the needle position must be adjusted before injecting.
Specific Joint Injection Sites
Successful joint injections rely heavily on accurate anatomical knowledge and precise targeting. The fetlock joint, commonly affected by osteoarthritis, requires careful palpation to locate the dorsal or palmar recesses. Carpal (knee) joint injections involve multiple compartments, demanding a thorough understanding of the joint’s complex structure;
Similarly, the tarsal (hock) joint presents challenges due to its limited space and multiple ligaments. Stifle joint injections necessitate precise needle placement to avoid neurovascular structures. Each site demands a unique approach, considering anatomical landmarks and potential complications. Proper technique minimizes risk and maximizes therapeutic benefit.
7.1 Fetlock Joint Injections
Fetlock joint injections are frequently performed due to the high incidence of osteoarthritis in this region. The dorsal and palmar/plantar recesses are the primary targets for injection. Palpation is crucial to accurately identify these recesses, often aided by transillumination. A sterile approach, utilizing appropriate needle length and gauge, is paramount.
Care must be taken to avoid superficial digital flexor tendon and pastern joint. Post-injection, horses typically require a period of controlled exercise to distribute the medication. Complications, though rare, can include infection or localized swelling. Careful monitoring is essential for optimal outcomes and to ensure the horse’s comfort.
7.2 Carpal (Knee) Joint Injections
Carpal joint injections target the complex anatomy of the horse’s knee, addressing issues like osteoarthritis and synovitis. Several recesses exist – the medial, lateral, and intermediate – requiring precise needle placement guided by anatomical knowledge and palpation skills. Ultrasound guidance is increasingly utilized for enhanced accuracy.
Sterile technique is critical, given the proximity to tendons and ligaments. Post-injection protocols typically involve a period of stall rest followed by a gradual increase in exercise. Potential complications include infection, though this is uncommon with strict aseptic practices. Monitoring for swelling or lameness post-procedure is vital for successful management.
7.3 Tarsal (Hock) Joint Injections
Tarsal (hock) joint injections are frequently performed due to the hock’s susceptibility to osteoarthritis, particularly in performance horses. The hock presents multiple synovial compartments – the proximal, middle, and distal – each potentially requiring individual attention. Palpation skills are essential to identify these compartments and guide needle placement accurately.
Ultrasound guidance is often employed to confirm correct positioning and minimize the risk of injecting surrounding tissues. Following injection, a period of controlled exercise is generally recommended, avoiding strenuous activity initially. Careful monitoring for any signs of reaction, such as increased heat or swelling, is crucial for optimal outcomes.
7.4 Stifle Joint Injections
The stifle joint, analogous to the human knee, is a complex structure prone to various issues requiring injection therapy. Medial and lateral femorotibial joints, as well as the femoropatellar joint, comprise the stifle, and can be injected separately or concurrently depending on the diagnosis. Accurate stifle joint injections demand a thorough understanding of the anatomy and careful palpation.
Ultrasound guidance is highly recommended for stifle injections, given the surrounding musculature and potential for misdirection. Post-injection protocols typically involve a period of controlled walking exercise, gradually increasing intensity as tolerated. Monitoring for swelling, heat, or lameness is vital to assess treatment efficacy and identify potential complications.
Post-Injection Care & Rehabilitation
Following a joint injection, a carefully managed rehabilitation program is crucial for optimal outcomes. Initial rest, typically 24-72 hours, allows the medication to take effect and minimizes inflammation. Controlled exercise is then gradually introduced, starting with hand-walking and progressing to trotting and cantering as tolerated. The duration and intensity of exercise are tailored to the individual horse and the injected joint;
Regular monitoring for signs of pain, swelling, or heat is essential. Cold therapy, such as icing, can help reduce inflammation during the initial phase. Maintaining a consistent exercise schedule and avoiding strenuous activity too soon are key to successful rehabilitation and long-term joint health.
Potential Complications & Side Effects
While generally safe, equine joint injections carry potential risks. Infection (septic arthritis) is a serious, though rare, complication requiring immediate veterinary attention. Corticosteroid injections, while effective, can increase the risk of laminitis, particularly in horses prone to the condition; careful monitoring of hoof health is vital.
Local injection site reactions, such as mild swelling or discomfort, are common and usually resolve quickly. Systemic side effects from corticosteroids can include increased thirst and urination. It’s crucial to report any concerning signs to your veterinarian promptly for appropriate management and to ensure the horse’s well-being.
9.1 Infection (Septic Arthritis)
Septic arthritis represents a critical complication following joint injection. This occurs when bacteria contaminate the joint space, leading to severe inflammation and potential joint damage. Symptoms include dramatic swelling, heat, pain, and often, a complete unwillingness to bear weight. Immediate veterinary intervention is paramount, typically involving joint lavage (flushing) and aggressive antibiotic therapy.
Strict adherence to sterile technique during injection is the primary preventative measure. Early recognition and prompt treatment are crucial to minimize long-term consequences, which can include cartilage destruction and permanent lameness. Prognosis varies depending on the severity and duration of the infection.
9.2 Laminitis Risk (Corticosteroids)
Corticosteroid injections, while effective for joint inflammation, carry a potential risk of triggering laminitis, a painful condition affecting the laminae within the hoof. This risk is particularly elevated in horses predisposed to endocrine disorders like Cushing’s disease or Equine Metabolic Syndrome. The mechanism isn’t fully understood, but involves disruption of normal blood flow to the hoof.

Careful consideration of the dosage, frequency of injections, and the horse’s overall health status is vital. Monitoring for early signs of laminitis – increased digital pulse, heat in the hooves, and reluctance to move – is crucial. Prophylactic hoof support may be recommended in at-risk individuals.
9.3 Injection Site Reactions
Localized reactions at the injection site are relatively common following equine joint injections. These typically manifest as mild swelling, heat, and transient pain, usually resolving within a few days. Strict adherence to sterile technique during injection minimizes the risk of more significant reactions.
However, more pronounced reactions, including cellulitis (bacterial infection of the skin) or seromas (fluid accumulation), can occur. Careful monitoring of the injection site post-procedure is essential. Contact your veterinarian immediately if you observe excessive swelling, discharge, or prolonged lameness. Cold hosing can help manage mild inflammation.
Cost Considerations for Joint Injections
The cost of equine joint injections varies significantly based on several factors. These include the type of medication used (corticosteroids being generally less expensive than biologics like IRAP or stem cells), the veterinarian’s fees, and the number of joints injected. A single corticosteroid injection might range from $200-$500, while biologic therapies can easily exceed $1,500 per joint.
Diagnostic procedures, such as radiography or ultrasound, add to the overall expense. Furthermore, post-injection care, including bandaging and rehabilitation, incurs additional costs. Discuss a detailed estimate with your veterinarian before proceeding to understand the full financial commitment.
Long-Term Management & Prevention
Joint injections are often part of a broader, long-term management plan, not a standalone cure. Maintaining optimal body condition, regular controlled exercise, and appropriate farrier care are crucial for supporting joint health. Consider incorporating joint supplements containing glucosamine, chondroitin, and omega-3 fatty acids into the horse’s diet.
Proactive management includes identifying and addressing risk factors like conformation flaws or previous injuries. Regular veterinary check-ups and early intervention at the first signs of lameness can help prevent further joint deterioration. A holistic approach focusing on prevention is key to maximizing a horse’s athletic longevity.